| Table of Contents |  |
|
Case Series
| |||||
| Residual periarticular complications of chikungunya virus infection in Mauritius | |||||
| Khadijah Dawood Essackjee1, Smita Goorah2 | |||||
|
1MPhil, University of Mauritius – MPhil graduate, Department of Medicine, University of Mauritius.
2MRCP, University of Mauritius – Associate Professor, Department of Medicine, University of Mauritius. | |||||
| |||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article: |
| Essackjee KD, Goorah S. Residual periarticular complications of chikungunya virus infection in Mauritius. J Case Rep Images Med 2016;2:44–49. |
|
Abstract
|
|
Introduction:
The tropical island of Mauritius has experienced two mosquito-borne chikungunya fever outbreaks in recent years. Acute symptoms of chikungunya fever are well described and commonly include an acute onset fever, severe arthralgia and rash accompanied by myalgia and headache. In most cases, there is complete resolution of symptoms. However, residual joint symptoms such as persistent polyarthralgia, joint stiffness, joint swelling and joint effusion have been reported in literature. Residual periarticular features are less well-known. Residual articular and periarticular manifestations were investigated more than two years after initial chikungunya infection in a selected cohort of affected people in Mauritius.
Case Series: Herein, we presented three clinical cases which describe interesting residual periarticular features post-chikungunya infection. These features include the manifestation of a swelling near the ankle joint, the persistence of a subcutaneous nodule near the wrist joint, the manifestation of tenosynovitis and the development of a prominent bony knee swelling in patients. Conclusion: Periarticular manifestations are seen more than two years after chikungunya fever suggesting persistence of long-term sequelae. | |
|
Keywords:
Chikungunya virus, Clinical case reports, Musculoskeletal complications, Residual periarticular complications
| |
|
Introduction
| ||||||
|
Chikungunya virus (CHIKV) is the causative agent of chikungunya fever, several outbreaks of which have been reported in Africa, Asia and Europe and, as from late 2013, in the Americas [1] resulting in a significantly large number of cases worldwide [2]. CHIKV, an alpha virus of the Togaviridae family, is transmitted to humans by mosquitoes of the Aedes species. Acute symptoms of chikungunya fever are well described and commonly include an acute onset fever, severe arthralgia and rash accompanied by myalgia and headache [3]. Although chronic joint complications post-CHIKV infection has frequently been reported in literature, features of residual periarticular soft tissue and musculoskeletal complications are less well-known. The earliest reports of chronic articular and periarticular complications following CHIKV infection have been by Fourier and Morrison [4], by Kennedy et al. [5] and by Brighton et al. [6]. In recent years, researchers have frequently reported chronic joint manifestations months or years post-CHIKV infection [7] [8][9][10][11] [12][13][14][15][16] [17][18][19]. These features include persistent polyarthralgia and/or polyarthritis [7] [8][9][10][11][12][13][14][15][16][17][18][19], joint stiffness or morning stiffness [7] [8] [10][12][15][16] [18], joint swelling [7] [8][9][10][11][12] [13] [15] [19][16] and joint effusion [8] [12]. Radiological features have included bone erosions [11] [12] and joint space narrowing [11] [18]. Pain is a recurrent feature and includes, in addition to polyarthralgia in affected joints, osteoligamentous pain [15], exacerbation of pain in previously injured joints [8], soft tissue aches and pains [14] and myalgia [12] [15]. Other residual features described in literature have included tenosynovitis [7] [8][12][13][14] bursitis [13], nerve compression in the carpal, tarsal or cubital tunnels [7][8] [18], Raynaud's phenomenon [7][8] and subcutaneous nodules [16]. Fixed flexion deformity of the proximal interphalangeal joint has also been reported [12] . The tropical island of Mauritius in the Indian Ocean has experienced two chikungunya fever outbreaks with approximately 3600 and 11000 cases in 2005 and 2006 respectively [20]. In a study carried out 27.5 months after initial CHIKV infection on 173 individuals diagnosed using clinical criteria in an epidemic situation, 136 still had persisting joint and muscle symptoms of varying nature and intensity [16]. These manifestations were: joint pain at rest, joint pain on exertion, joint swelling, nodules near joints, joint deformity, morning stiffness, muscle weakness, paraesthesias and lymphadenopathy. The ankles and other joints of the feet were the most affected joints whilst the least affected one was the elbow. Further to the study [16], we had concluded that persisting symptoms were associated with older age at time of infection, female gender and baseline symmetrical distribution of joint symptoms. In addition, we had observed that 5% of those infected with CHIKV fulfilled a modified version of the American College of Rheumatology criteria for rheumatoid arthritis 27.5 months after infection. At the time of the study [16], visual evidence of the aftermath of CHIKV had also been collected with informed written consent obtained from the participants for the use of the clinical images. The aim of the present report is to describe a series of three clinical cases with residual periarticular features associated with CHIKV which are of particular interest. | ||||||
|
Case Series
| ||||||
|
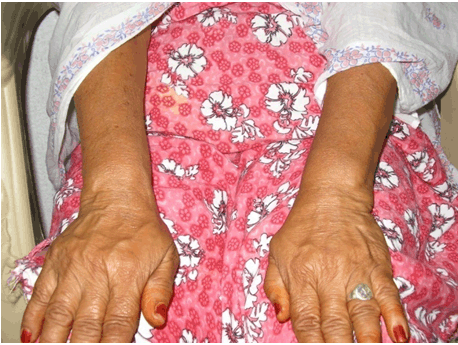
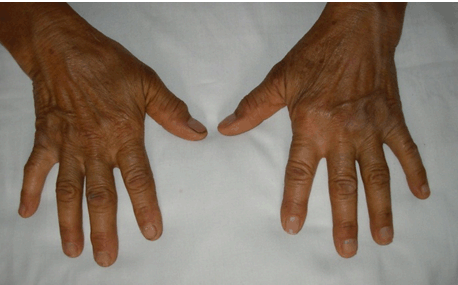
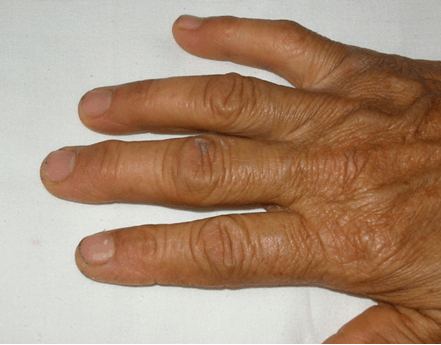
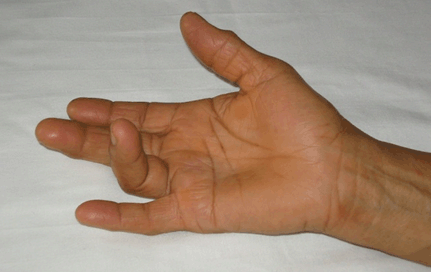
Case 1 Regarding the upper limbs of the patient in Case 1, it was observed that the small joints of the left hand were more swollen than those of the right hand. In addition, there was a visible nodule which was firm and subcutaneous and was located at the left wrist. The patient also complained of a residual stiffness in the left hand. These features were not present before the CHIKV infection. A comparison of both hands is shown in Figure 3. The swollen joints indicate residual periarticular and articular swelling of the small joints of the left hand and the nodule had a similar appearance to a rheumatoid nodule. Case 2 However, the most significant residual manifestations affected her hands. There was joint stiffness and restriction of movements in both hands with her right hand being more affected. Figure 4 shows the comparison between the right and left hands and it can be observed that the joints of the right hand appear more swollen than those of the left hand. Initially the small joints of both hands were very swollen during the acute phase of the infection. After the initial inflammation subsided, the patient noted that the appearance of her right hand had changed significantly due to joint swelling and this change was apparent more than two years after initial infection. Figure 5 shows the dorsum of the right hand. There is a noticeable nodule on the distal interphalangeal joint of the third digit. This nodule appeared shortly after the CHIKV infection. In May 2007, the patient suffered from an inability to extend the fourth digit of the right hand. This was resolved with the oral intake of non-steroidal anti-inflammatory drugs (NSAIDs). However in October 2010, the condition recurred and did not resolve with oral NSAIDs. A diagnosis of stenosing tenosynovitis Figure 6 was made. Subsequently, an injection of NSAIDs in the tendon sheath just beneath the finger enabled the patient to regain the use of her finger soon afterwards. Case 3 | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
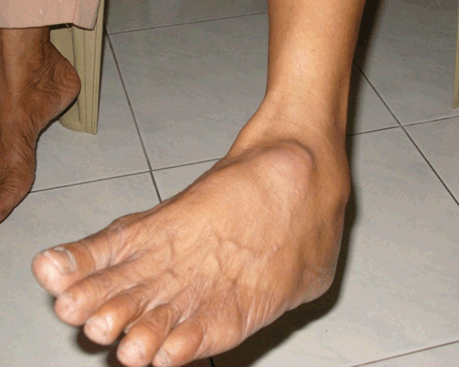
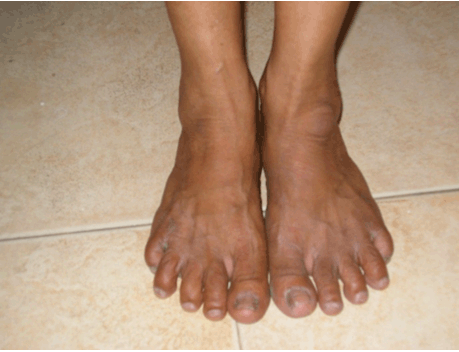
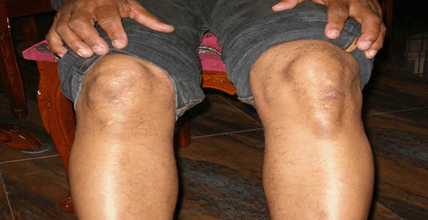
These three clinical cases describe residual periarticular features in patients more than two years after a clinical diagnosis of chikungunya fever. In all cases, patients have described features which manifested after the resolution of acute symptoms of chikungunya fever. Strikingly, the patients have described these particular manifestations as being strongly associated with the infection; they were non-existent before the infection and evolved as continuity from the acute symptoms. Such clinical manifestations suggest visible signs and sequelae of chronic inflammation. In Case 1, it is observed that the patient suffers from a swelling near the ankle joint most likely due to a ganglion cyst which is a fluid filled mass associated with tendon sheaths or joint capsules. Bursitis has previously been reported in literature as a complication of CHIKV infection [13] but to our knowledge there are no reports of ganglion cysts being associated with the infection. It is possible that injury to the joint or tendon sheath caused by inflammation during the acute phase of the infection has led to the formation of the ganglion cyst. It would have been advisable to investigate the swelling further by ultrasound scan or MRI scan to establish a definitive aetiology, however in this case the diagnosis was made clinically. As for the nodule on the patient's left wrist, this is consistent with findings of the study where we reported that 7% of participants with long term CHIKV complications reported joint nodules [16]. As in Case 2, tenosynovitis has been reported to be associated with CHIKV infection in several published articles [7][8] [12][13][14]. Stenosing tenosynovitis is a condition which arises when there is inflammation in flexor tendon sheath causing difficulty in straightening the affected finger. Clinical evidence of tenosynovitis associated with CHIKV infection had been reported by Kennedy et al. as early as 1980 [5]. It has also been reported by Parola et al. in recent times [8]. This finding is also supported by MRI studies [12]. Hence, there is evidence to show that tenosynovitis is a recognised residual manifestation of CHIKV infection. The prominent tibial tuberosity seen in the patient in Case 3 after CHIKV infection has not been reported in literature. Usually such a feature is usually seen in Osgood-Schlatter disease in young adolescents and is caused by an inflammation of the patellar ligament at the tibial tuberosity. In this case, it is plausible that the prominent tibial tuberosity is a sequel of tendinitis caused by the infection. There is need for clear guidelines for the specific management of post-CHIKV musculoskeletal complications. This has also been highlighted in a recent publication [18]. All the cases described in this report were treated conservatively in the community. | ||||||
|
Conclusion
| ||||||
|
Evidence has gradually been emerging regarding periarticular sequelae post-chikungunya fever. The clinical cases described give additional evidence of some sequelae involving mostly periarticular structures such as tendons. The clinical cases also show that sequelae are present more than two years after initial infection with CHIKV. Further studies are required to investigate the full range of articular and periarticular residual symptoms. | ||||||
|
Acknowledgements
| ||||||
|
We would like to thank the Tertiary Education Commission, Mauritius for providing a postgraduate scholarship for this research. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Khadijah Dawood Essackjee – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Smita Goorah – Substantial contributions to conception and design, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Khadijah Dawood Essackjee et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|