|
|
Clinical Image
| ||||||
| The morning after rash: Erythema nodosum due to emergency contraception | ||||||
| Charlotte Andrews1, Jacob Mathew2 | ||||||
|
1Aviation Physician Assistant, Department of Aviation Medicine, Evans Army Community Hospital, Fort Carson, CO, USA 2Flight Surgeon, Department of Aviation Medicine, Evans Army Community Hospital, Fort Carson, CO, USA | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in PubMed] [Similar article in Google Scholar] |
| How to cite this article |
| Andrews C, Mathew J. The morning after rash: Erythema nodosum due to emergency contraception. J Case Rep Images Med 2018;4:100045Z09CA2018. |
|
CASE REPORT
| ||||||
|
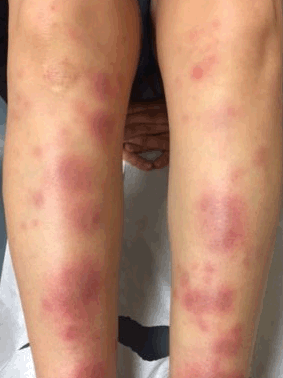
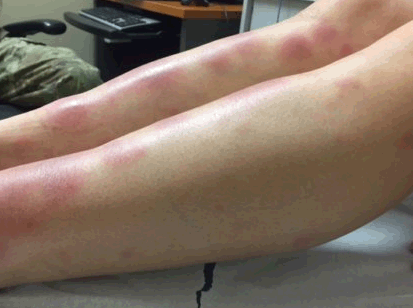
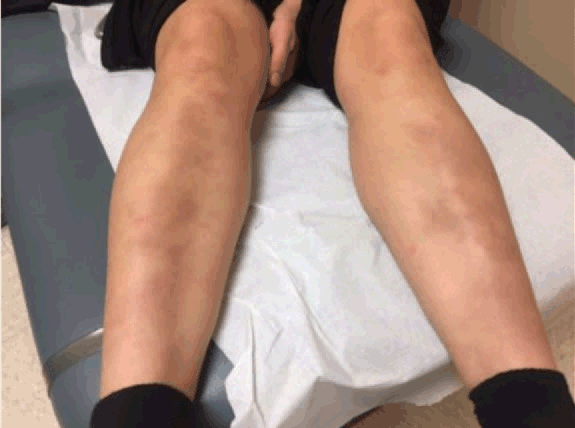
A 19-year-old Caucasian female in the United States Army with an unrevealing past medical history presented due to the sudden onset of painful nodules and bruising to her on shins that developed upon awakening two days ago. She denies recent trauma to the area. No recent upper respiratory infections. No family history of sarcoidosis, rheumatoid arthritis, or other autoimmune conditions. She described the pain as a burning sensation. She denies spread of the lesions since they first appeared. She denies a history of similar symptoms in the past. She does not take any chronic medications but does admit to taking a form of emergency contraception after unprotected sexual intercourse, approximately one week prior to their appearance. Denies any joint pains. On physical examination, vitals were stable with no evidence of fever. The patient was in no acute distress. Cardiopulmonary examination was unremarkable. Skin examination revealed ill-defined symmetric subcutaneous nodules, approximately 4–5 cm in size, with bruising on the anterior shins bilaterally (Figures 1 and 2). Examination of the ankles, knees, elbows, and fingers bilaterally showed no evidence of synovitis. Elevated Sedimentation Rate (ESR) was 37 mm/hr (normal range for women 0-29 mm/hr). Erythema nodosum (EN) was highest on the differential diagnosis, and the patient was referred to Dermatology for clinical confirmation of the diagnosis. Given its appearance, Dermatology confirmed the diagnosis, and biopsy was not pursued. She was prescribed a prednisone taper of 20mg for 21 days. Upon follow up a month later, her symptoms had mostly resolved as seen in attached figures (Figures 3 and 4). Keywords: Erythema nodosum, Emergency contraception, Panniculitis | ||||||
|
DISCUSSION
| ||||||
|
Erythema nodosum is a form of panniculitis, more commonly seen in females, that can be associated with a wide breadth of conditions (Table 1). Oral contraceptives, as well as many other conditions, have been associated with erythema nodosum [1], [2]. EN often produces painful ill-defined symmetric subcutaneous nodules, often 1–6 cm in diameter, in areas such as the face, neck, trunk or arms but most commonly seen in the anterior surface of the lower extremities [3], [4], [5], [6]. The nodules will often regress to bruises and ultimately will disappear without bruising in 1–2 months [3]. In rare cases, the dermatologic manifestations may be associated with systemic symptoms of fevers, malaise, and joint pains [6]. EN may be a sign of an underlying medical condition such as inflammatory bowel disease, sarcoidosis, malignancy, specific bacterial infections, or from medications such as oral contracptives, sulphonamides or bromides [7]. Table 1 shows common causes of Erythema nodosum [4],[6],[7]. Despite the large differential, malignancy must always be considered as a potential cause. A paraneoplastic presentation can be seen with Non-Hodgkin’s lymphoma, Hodgkin’s lymhpma, and leukemia [6]. Diagnosis can often be made solely on patient history and physical examination. Dermatologic exam often reveals an acute onset of tender nodules on the bilateral shins. Biopsy can be considered if an atypical site is involved (ie. arms, chest) or atypical features are encountered such as ulceration or abnormally large size (>5 cm). Typically labs are not necessary unless they may assist in the diagnosis of the culprit disease (i.e. chest radiograph for sarcoidosis, ESR or C-RP for inflammatory bowel disease). Treatment is often conservative and involves raising the legs, rest, anti-inflammatories, and systemic glucocortidoids, if rapid treatment is desired. CO | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
CONCLUSION
| ||||||
|
Erythema nodosum is a dermatologic condition that may present with nodular erythematous eruptions that is usually limited to the extensor aspects of the extremities in patients secondary to a wide array of potential conditions as well as secondary to medications. Oral contraceptives are a known, but not commonly considered cause, of EN, and should be considered in the differential in age-appropriate females presenting in the right clinical scenario with painful nodules and bruising to the lower extremities. Treatment is often conservative, however, in severe cases, prednisone can be used. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Charlotte Andrews – Acquisition of data, Revising it critically for important intellectual content, Final approval of the version to be published Jacob Mathew – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of Submission
The corresponding author is the guarantor of submission. |
|
Source of Support
None |
|
Consent Statement
Written informed consent was obtained from the patient for publication of this clinical image. |
|
Conflict of Interest
This article was prepared or accomplished by Charlotte Andrews and Jacob Mathew in their personal capacity. The opinions expressed in this article are the author’s own and do not reflect the view of the United States Army, the Department of Defense, or the United States government. Neither author has any conflicts of interest to report. |
|
Copyright
© 2018 Charlotte Andrews et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|